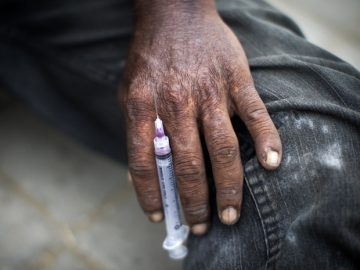
 The Hotel Study is a 10 year longitudinal CIHR-funded investigation of public health issues in Vancouver’s Downtown Eastside (DTES) that focuses on the intersection of physical and mental health, along with the relationship to drug addiction and access to public health systems.
The Hotel Study is a 10 year longitudinal CIHR-funded investigation of public health issues in Vancouver’s Downtown Eastside (DTES) that focuses on the intersection of physical and mental health, along with the relationship to drug addiction and access to public health systems.
Around the world and close to home, health and wellness are experienced on a social gradient. Consistently, those with lower socioeconomic position experience worse health. Mental illness and addictions are linked with social inequities including poverty, stigma, and social exclusion.
In Vancouver’s DTES neighbourhood, poverty, trauma, illness, and substance use are unfortunately prevalent among its residents. Substantial health research has engaged the DTES community to reduce overdose deaths, transmission of HIV, and to test addiction treatment and housing approaches, however these interventions have had limited impact on daily substance use and mental health. Unaddressed mental health issues can lead to devastating consequences and can lead to involvement with the criminal justice system and further exacerbation of barriers to wellness.
Overall, the impact of mental illness in the community is largely unstudied and requires attention.
To address this gap, the Hotel Study was launched to better characterize the health needs of the DTES population, with a particular focus on mental health and cognitive function. This naturalistic, longitudinal observational study follows over 400 adults living in marginalized housing. The study comprehensively investigates mental, physical, and social health domains over ten years to better understand the intersecting biological, psychological, and social effects of factors affecting mental health.
The Hotel Study has identified a high prevalence, and significant impact, of mental illness among marginally housed adults in Vancouver’s DTES. Mental illness contributes to the compounding health challenges and premature mortality faced by these individuals. The high rates of mortality, multimorbidity (the co-occurrence of two or more chronic medical conditions in one person), and cognitive impairment suggests an accelerated aging process experienced by these adults who are marginalized by complex illness, poverty, and other social inequities.
These challenges may impact the accessibility and quality of care received, which is something our health system must prepare for these complex needs to improve quality of life and wellness among this population.